Tethered spinal cord syndrome
Tethered spinal cord and spinal dysraphism in children: general information
Spinal dysraphisms ( from the Greek dys = bad, raphe = closure, suture) include a large group of pathologies with variable severity (spina bifida occulta, diastematomelia, lipomeningocele, meningocele, myelomeningocele , caudal regression syndrome) in which there is a developmental anomaly involving the vertebral column and spinal cord (due to an alteration in the closure of the “neural tube”).
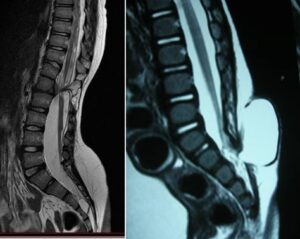
This results in a wide variety of pathological conditions, from milder forms of spina bifida occulta (failure of one or more vertebral arches to fusion, which may be an occasional finding with no pathological significance) to forms of caudal regression syndrome (sacral and lumbosacral agenesis) characterized by the absence of variable portions of the lumbar and sacral spine (and the corresponding nervous structures), up to severe forms of myelomeningocele in which severe involvement of the nervous structures is evident from birth (motor paralysis, sensitivity disorders, sphincter disorders, hydrocephalus, etc.).
A common feature of spinal dysraphism is the close connection between orthopedic and neurological problems: the latter must therefore be carefully considered in the treatment (physiotherapy, orthotics, surgery) of these patients.
Orthopedic problems of spinal dysraphism
While the most severe forms of spinal dysraphism (myelomeningocele, caudal regression) are always evident at birth and require early intervention by a multidisciplinary team, other forms (lipomeningocele, diastematomelia, etc.) may be completely asymptomatic at birth and in the first few years of life, and may present for orthopedic evaluation during growth due to the onset of progressive musculoskeletal changes.
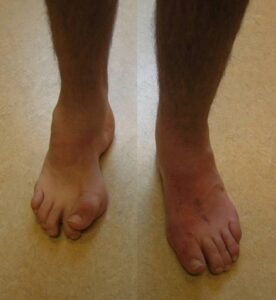
In these conditions, the underlying malformation causes progressive disruption of the nervous structures (spinal cord, nerve roots) with growth, resulting in peripheral neurological deficits and progressive deformations of the lower limbs.
This generally occurs due to the spinal cord becoming tethered to surrounding structures at the level of the malformation, which, as the patient grows, leads to progressive stretching of the cord itself.
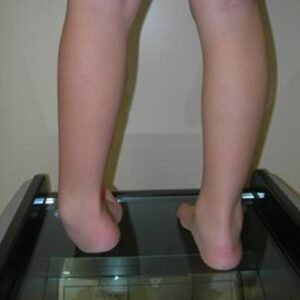
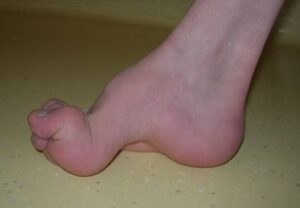
The orthopedic surgeon’s task is to suspect that these deformities are secondary to spinal dysraphism and initiate investigations (electrophysiological tests, MRI, etc.) for these pathologies.
Sometimes the presence of skin alterations (angiomas, skin dimples, tufts of hair, lipomatous masses, etc. ) in the midline of the lumbar or lumbosacral region can help raise suspicion of these pathologies. But above all, it is essential to perform a careful clinical evaluation with a thorough neurological examination, which must highlight any neurological deficits present (muscle weakness, sensory alterations, sphincter disorders).
The patient will then be referred for a neurosurgical evaluation , for a possible intervention to free the nervous structures, with the aim of removing, if possible, the underlying causes of the orthopedic problem or at least limiting its progression.
Once the neurosurgeon’s opinion has been obtained, surgical correction can be planned. However, deformities associated with spinal dysraphism carry a high risk of recurrence with growth, due to underlying neurological imbalances.
Patients from abroad: can OrthoChildren Center treat foreign patients?
Yes, many patients come from all countries (Europe and USA):
- the surgical equipe has a wide experience with this condition
- An intensive rehabilitation program can be included
- the procedure is less expensive than in USA and other countries
- Families take advantage of this opportunity to combine a trip to the beauties of Italy
